Webinar
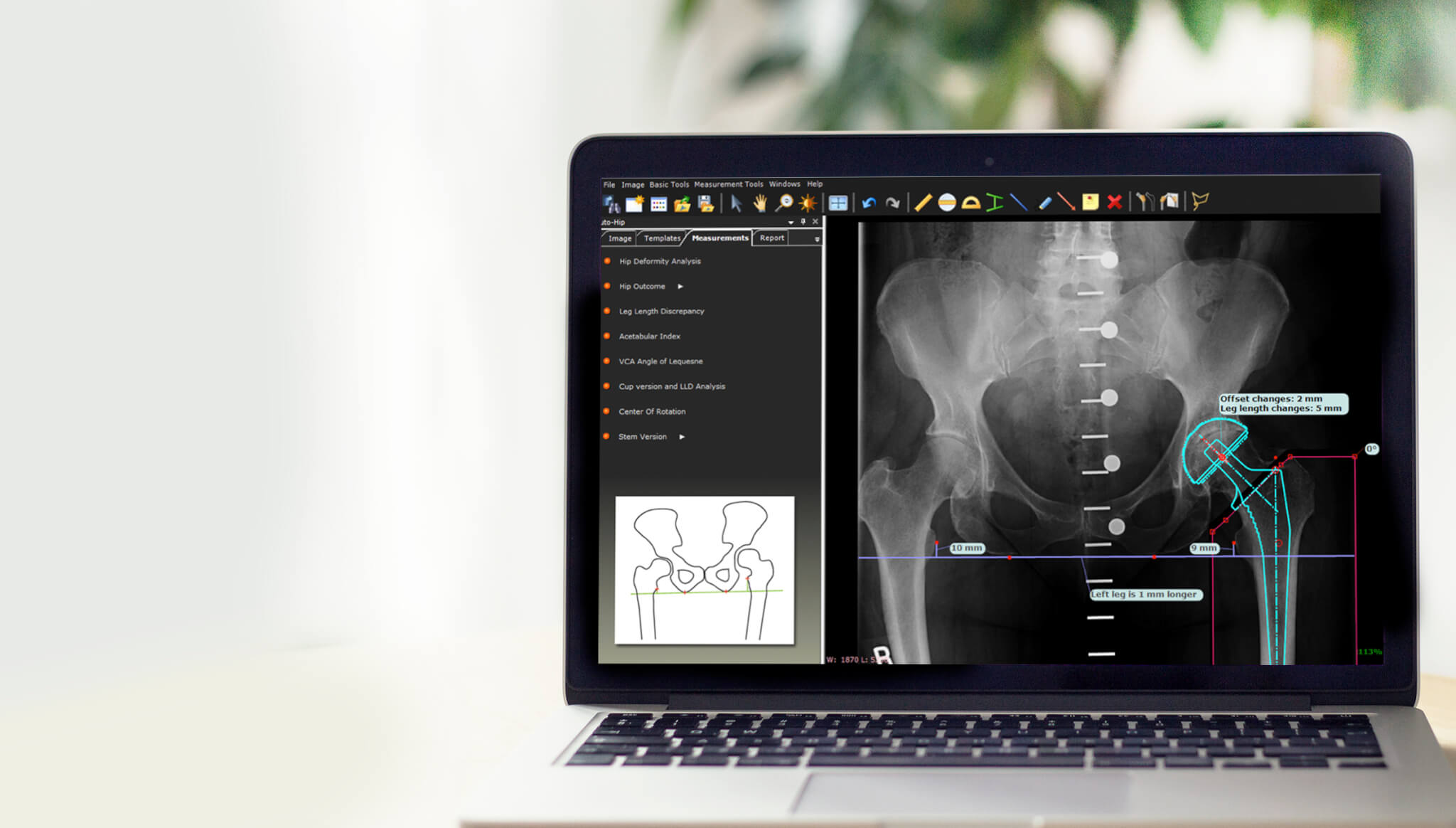
TraumaCad Fundamentals
Beschreibung
Brainlab invites you to join our webinar, “TraumaCad Fundamentals”, on November 24, 2020 presented by Ian Wilson, Sales Manager TraumaCad International.
Learn the fundamentals of pre-op planning with TraumaCad for Total Hip Replacement, Total Knee Replacement, and Deformity correction. Join us for a training session, provided by the TraumaCad experts.
The views, information and opinions expressed within this presentation are from the speakers and do not necessarily represent those of Brainlab.
Sprecher:in:

Ian Wilson, Sales Manager TraumaCad International
Moderator:in:

Chen Bacharuzi, Junior Marketing Manager, TraumaCad
Weitere Webinare anzeigen
Jetzt anmelden