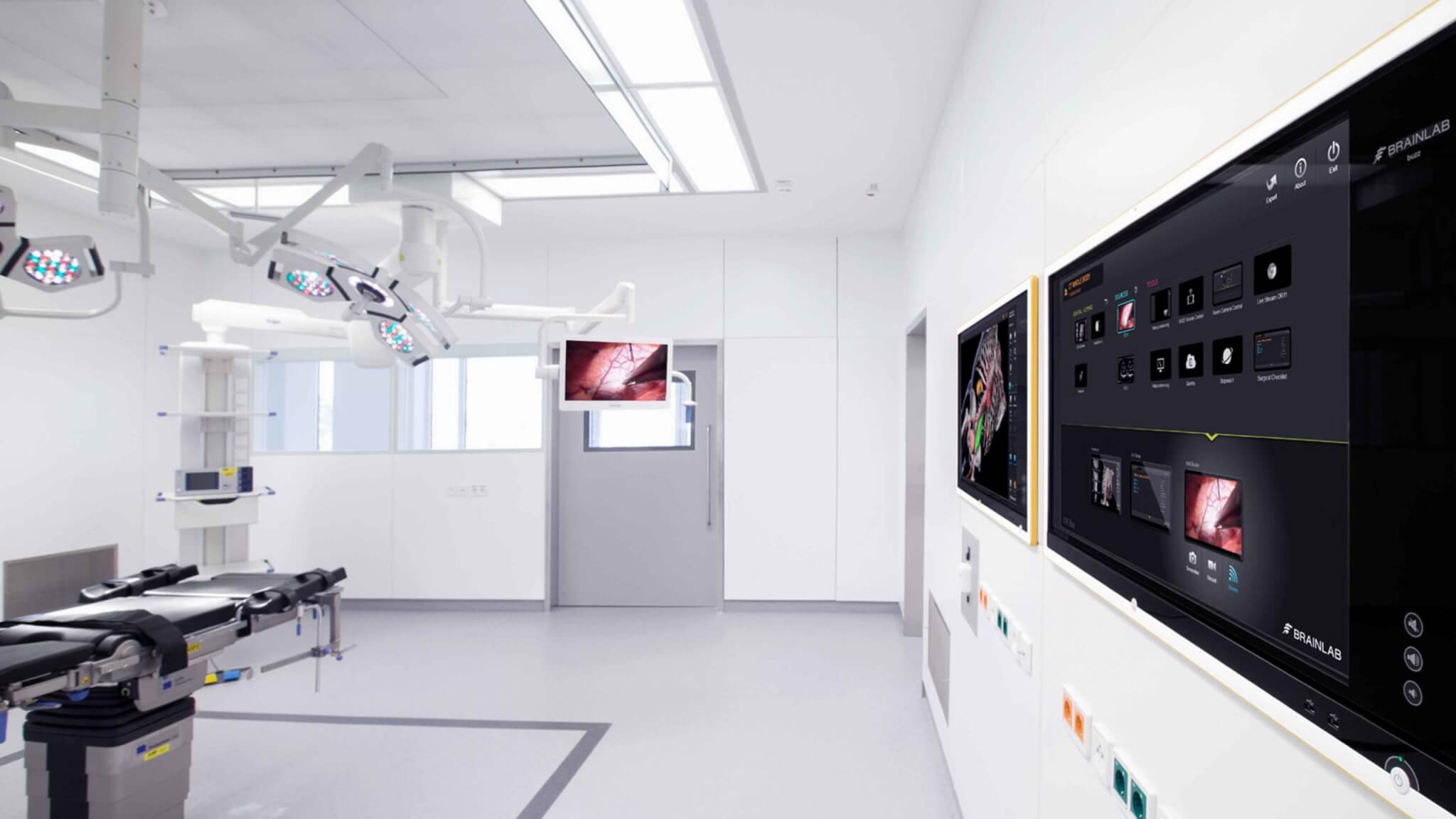
It seems that nowadays there are hundreds of buzz words to describe digital operating room integration but very few solid answers about what they all mean
When tasked with upgrading or even creating an integrated operating room environment, the sheer volume of buzzwords can be frankly overwhelming. What one hospital refers to as “O.R. integration” may mean something completely different in another country or even at the hospital down the street. That’s why we’ve put together the below to define operating room integration terms, describe the types of operating rooms and demystify the process of turning your analog O.R. into a well-oiled digital machine.
Before we can understand the meaning of each hybrid, integrated and digital O.R., we need to understand the basic operating room setup conventional, non-integrated operating room. First, before surgical procedure even begins, preoperative data has to be provided for each case and patient. Data is available either on paper or digitally on different devices that don’t talk to each other. Operating room machines and equipment are arranged around the room. Individual devices are pulled in or pushed back as needed. A nurse works with the equipment to adjust each device as required by the surgeon. Cables and cords lie everywhere on the floor, making it easier to trip, pull out an essential cord during surgery or damage the equipment.¹
With the addition of operating room integration systems to address these issues, a hospital can opt for what are sometimes interchangeably referred to as hybrid, integrated, or digital O.R. setups. While they may sound similar, the differences lie in the way the technology and data work together. In general, hybrid, integrated or digital operating rooms all share the common goal of improving safety to positively impact patient outcomes and simplifying workflows for the surgeon and surgical team.
What is a hybrid operating room?
Hybrid operating room requirements are usually based around imaging, like CT, MR, C-arm or other types of imaging, being brought into surgery. Bringing imaging into or adjacent to the surgical space means that the patient doesn’t have to be moved during surgery, reducing risk and inconvenience². Depending on the design of operating rooms in hospitals as well as their resources and needs, fixed or mobile hybrid operating rooms may be built. One-room fixed O.R.s offer maximum integration with a high-end MR scanner, allowing the patient to stay in the room, still anesthetized, during the scan. In two or three room configurations, the patient must be transported to an adjacent room for scanning, increasing the risk of inaccuracy through possible movement of the reference system. In O.R.s with mobile systems, the patient remains and the imaging system is brought to them. Mobile configurations offer different advantages, such as the flexibility to use imaging in multiple operating rooms, as well as generally lower costs, but may not provide the higher image quality a fixed imaging system could offer.
One further understanding of hybrid O.R.s is that they are multi-purpose rooms that are fitted to serve different surgical disciplines. With more and more complex procedures taking place, intraoperative imaging is certainly the future of surgery. Hybrid O.R.s generally focus on minimally invasive and vascular surgery. They are often shared by different surgical departments, such as vascular and spine.
Hybrid operating room benefits include scans of the affected part of the body being forwarded and available for review and use immediately in the operating room. This allows the surgeon to continue operating, for example, in a high risk area like the brain with the most up-to-date data.
What is an integrated operating room?
Integrated operating rooms were introduced in the late 90s as video routing systems capable of distributing video signals from one camera to multiple outputs or products became available. Over time, they evolved to be able to functionally connect the O.R. environment. Patient information, audio, video, surgical and room lights, building automation, and specialized equipment, including imaging devices, could all communicate with one another.
In some setups, when connected, all of these various aspects can be commanded from a central console by one operator³. Integrated O.R. is sometimes installed as a functional addition to an operating room to integrate the control of several devices from a single console and offer the operator more centralized access for device control.
What is a digital operating room?
In the past, a lightbox on the wall was used to display patient scans. A digital O.R. is a setup in which software sources, images and operating room video integration is made possible. All this data is then connected to and displayed on a single device. This goes beyond simple control of devices and software, allowing also for the enrichment of medical data within the operating room.
A digital O.R. setup therefore functions as a central hub for clinical image data inside the operating room and for recording, collecting and forwarding data to the Hospital IT system, where is it centrally stored. The surgeon can control the data inside the O.R. from specified displays according to their desired setup and also has the possibility to display the images from many different devices.
Before creating your O.R. of the future
While it is important to have a general idea of what these terms mean, the most important piece of the puzzle is knowing what your institution needs. Before you sit down to plan, meet with surgeons, nurses, operating room managers and other staff. Determine what hardware, software and workflows they need for their daily work and what their main goals for an advanced digital surgery room would be.
Be sure to also ask them what they foresee themselves needing in 5 or 10 years. If done right, a digitally integrated O.R. should be able to adapt and grow with the latest technological advances. If after all of that, you’re still feeling overwhelmed, seek the advice of an equipment planner or O.R. consultant. They will be able to point you in the right direction to make the best decision for the long-term success of your O.R. project!
1,3 Healthcare Design Magazine, The Integrated Operating Room, 2006