Webinar
Complex Case Discussion Focusing on Navigation and Image Fusion in Sinonasal Tumors
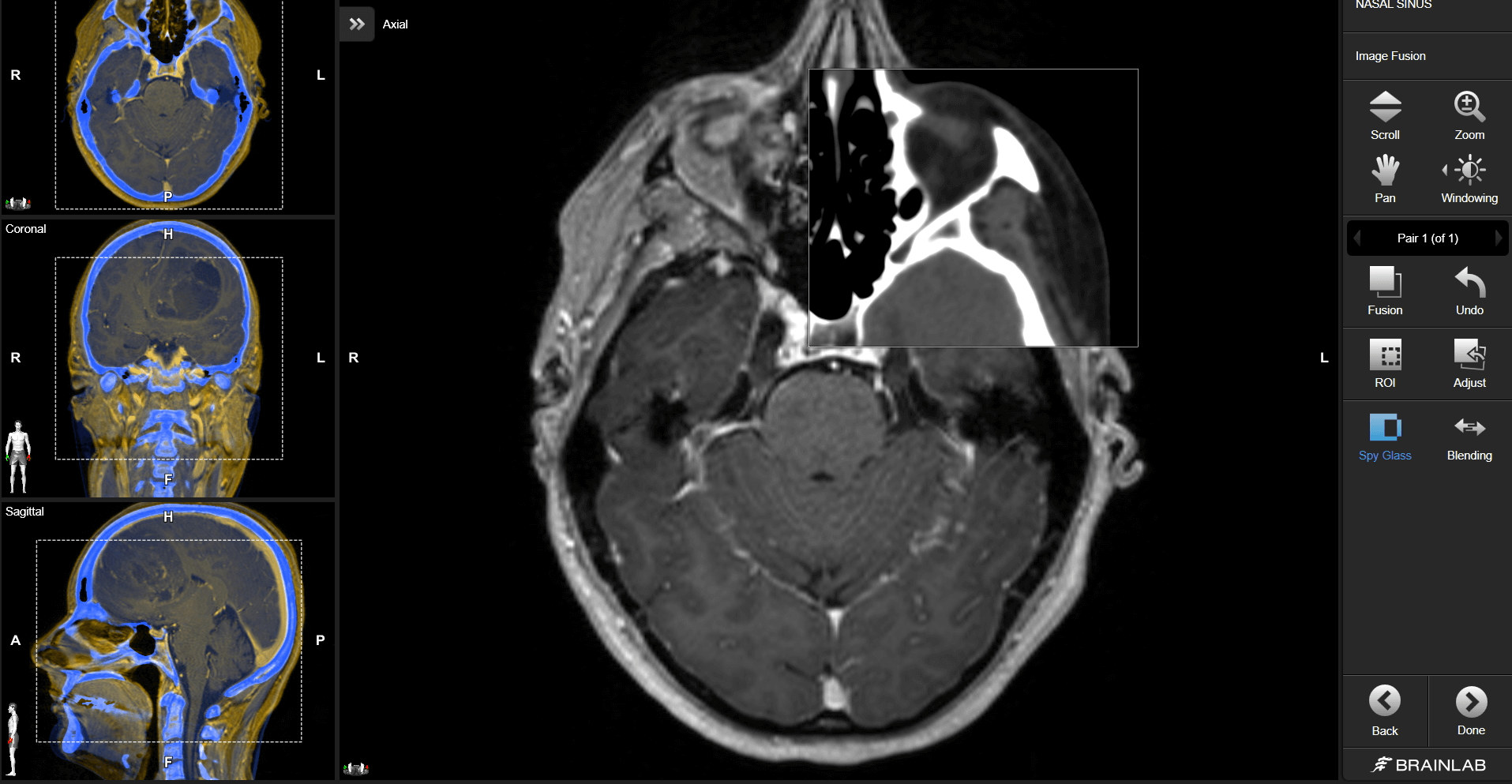
Description
Brainlab invites you to join a live webinar, “Complex Case Discussion Focusing on Navigation and Image Fusion in Sinonasal Tumors”. Taking place on March 10, 2021 at 4:00 PM CET, this webinar will be presented by Frank Haubner, MD, Senior Physician, Department of Otolaryngology, University Hospital Munich, Germany.
We look forward to meeting you online!
Language | English
In case you can’t join the webinar, it will be recorded and shared afterward.
Participation is free of charge.
The views, information and opinions expressed during this presentation are the speaker’s own and do not necessarily represent those of Brainlab.
Speaker:

Priv. Doz. Dr. med. Frank Haubner, Senior Physician, Department of Otolaryngology
University Hospital Munich, Germany, Munich, Germany
Moderator:

Jana Guggenberger, Director Product Management & Marketing Spinal/CMF Planning/Navigation
See more upcoming webinars
Discover more