How Digitalization Both Helps and Hinders Patient Communication
The most precious resource in the course of medical treatment is the doctor’s time. This resource, however, is becoming increasingly scarce due to the influx of amounts of data and the increasing effort required to document cases. This focus on data and documentation leaves less and less room for the empathic communication with the patient. Many approaches to solving this problem are concerned with the delegation of so-called non-medical tasks to other personnel, which makes sense for administrative tasks. For medical tasks, however, this leads to a further reduction of the direct contact between the doctor and the patient, instead of intensifying it.
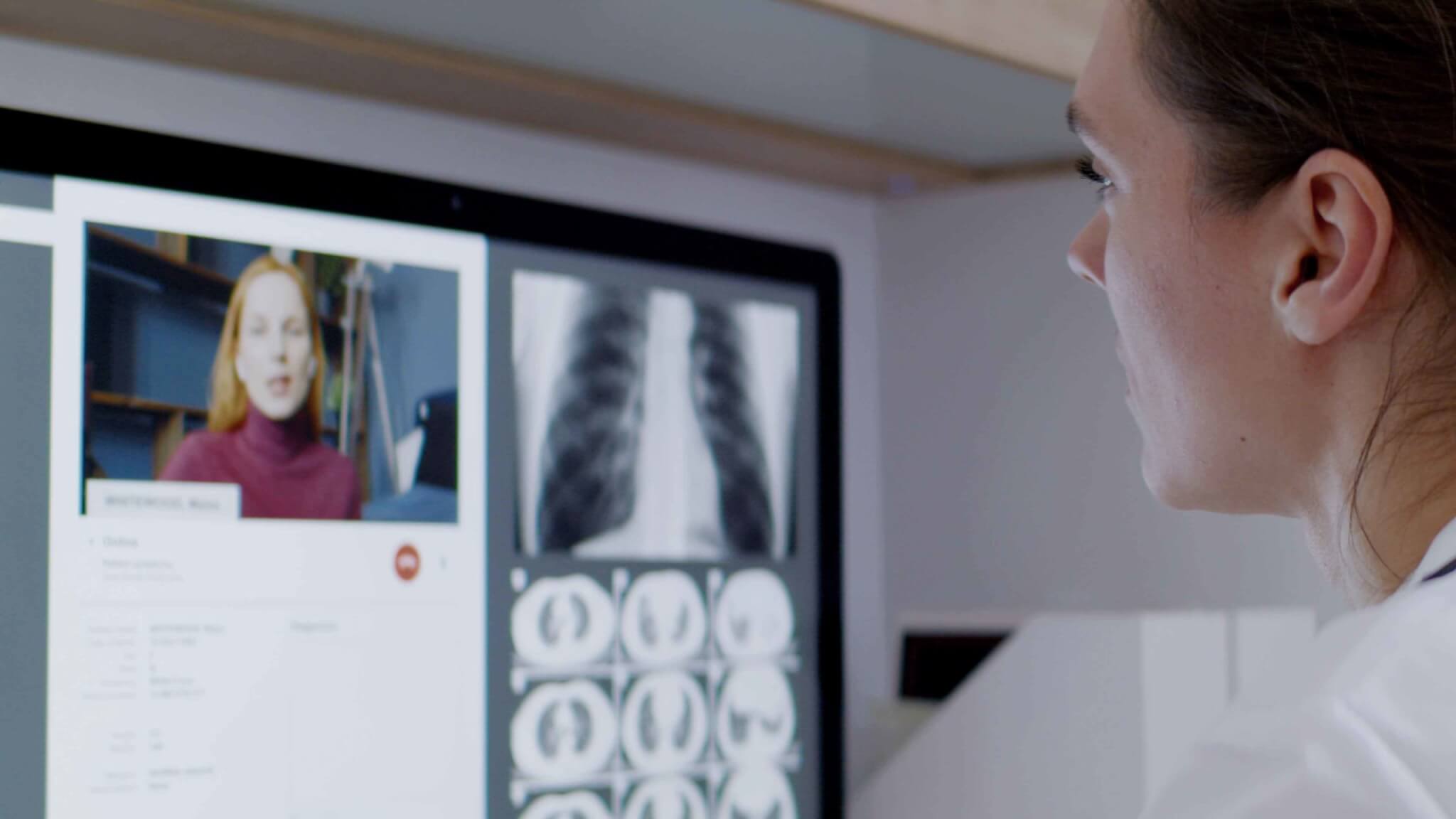
At first glance, it may seem astonishing that the increasing digitalization of medicine could be of service here. Today’s hospital information systems were primarily intended to be management software to facilitate administrative tasks. When the functionality of these systems was extended to include clinical documentation, the needs of physicians and nurses were largely ignored. These programs are therefore confusing and require a considerable amount of time to reach the necessary information. The core focus of the IT department, however, must be that the doctor can get all the necessary data for diagnosis and treatment faster and more efficiently, so that they don’t have to hide behind a computer in front of their patients. The computer should, rather, create space for constructive doctor-patient consultation.
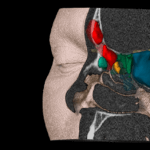
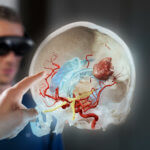
One example of software creating space for doctor-patient interaction is 3D visualization of radiological findings. These three dimensional images can not only create this space, but they can also significantly increase the quality of treatment. For example, many patients routinely come to follow-up on their tumor progression. Up until recently, many individual image series had to be called up from the digital patient file and laboriously compared with one another. Imagine now a 3D image with a time cursor, which, when shifted from left to right, automatically displays the changes over the course of time. Therapies that have taken place during that course of time are also included, in order to better understand changes in the treatment. At a glance, the doctor has more detailed and instantaneous information than available almost everywhere at present. From the perspective of the patient, they lose a little of their anxiety, because the less they are aware of their own illness, the more they feel dependent on the doctor.
In the over two years’ experience that I have with our 3D image viewer, our patients have clearly shown that they are better at understanding what their disease is and how the surgery they are about to have will take place. This reduces their uncertainty, creates confidence and reduces their fear of the unknown. Here, we are already seeing considerable improvement in physician-patient communication.
In the same way, it is also conceivable in the future to depict and understand other findings within a timeframe, for example, pain or paralysis in the course of treatment. I, therefore, see the future of patient consultation with digitally augmented visualization of the results, which makes the information more user-friendly, improves the content of the information, and relieves the physician of tasks that distract from the patient.
About the Author
Professor Veit Braun, MD, is the Head of Neurosurgery at the Jung-Stilling-Krankenhaus in Siegen, Germany. His work focuses on functional neuronavigation, especially relating to tumor resections in the brain, functional restoration of injury to the peripheral nerves and the treatment of aneurysms. He is a member of numerous societies including the German Society for Neurosurgery (Deutschen Gesellschaft für Neurochirurgie) and the German Society for Computer and Robot-assisted Surgery (Deutschen Gesellschaft für Computer- und Roboterassistierte Chirurgie).