It’s still relatively quiet at the Lokschuppen Museum in Rosenheim. On weekends and during school breaks, it’s much busier—especially when the weather’s bad. But today is Thursday, the sun is shining outside, and inside, Peter Miesbeck points to a watch on display. It belonged to a Swiss Titanic passenger. Recovered from his body, it was later returned to his family. “It shows the moment the ship went down—Swiss time,” Miesbeck says.
The Lokschuppen—once part of the Rosenheim train station grounds—has been a cultural exhibition center since 1988, with nearly 1,500m2 of gallery space. It’s just under an hour from Munich, though its exhibitions draw up to 280,000 visitors a year from far beyond the region. For more than 25 years, Peter Miesbeck served as the Lokschuppen’s director—and today, he’s one of two curators behind the 2025 exhibition: Titanic: Its Time. Its Fate. Its Myth.


“In just over two weeks, we’ve already had over 10,000 visitors,” he says, clearly pleased. The fact that he’s sitting here today, that he helped shape this exhibition in such a meaningful way—and most of all, that he can say, “I’m doing well”—is anything but a given after the past five years.
It was the summer of 2020. At the Lokschuppen, the exhibition Dinosaurs—Giants of the Sea was running under COVID restrictions when Peter Miesbeck, 59 years old at the time, sat down in his dermatologist’s office—just checking on a small, burning patch of skin on his temple. Nothing more. The doctor removed the patch and sent it off for testing. Then, in August 2020, the diagnosis came: malignant melanoma—skin cancer. More tests followed. So did more bad news. The cancer had already spread: metastases in the liver, the ribs, and the soft tissue.
“You can lie down and wait to die—or you can say to yourself: Take the chance.”

Online, Peter came across a number: “It said something about a 20 percent survival rate—and I thought, I’ll take it!” He approached his illness the way he would plan an exhibition: “I always saw it as a project—something you just have to manage. The most important thing is not to give up on yourself.”
The things that gave him strength throughout this particular project are, in the end, the same things he feels are worth fighting for:
Peter wanted to make the most of his chance—but at the same time, he was preparing for the worst. He divided his property and transfered ownership to his two sons. He pushed forward the search for new leadership at the Lokschuppen, eventually handing over his role to his successor in the summer of 2022. “You can’t pretend nothing’s happening—you have to get things in order,” he says. But his 26 years of exhibition planning have also taught him something else: “If you prepare well for all eventualities, most of them never actually happen.”
In the summer of 2020, despite the melanoma and metastases, Peter showed no physical symptoms. He began a targeted therapy. The medication works and the metastases in his liver and soft tissue begin to shrink. But new metastases develop in his brain where many medications are less effective due to the blood-brain barrier. In spring 2021, more than ten brain metastases were treated with targeted radiation. Afterward, an oncologist recommended whole-brain radiation.
“That was the last thing I wanted,” Peter says—his fear that critical areas of his brain could be damaged was simply too great.
“I still need my brain,” Miesbeck says with a laugh.

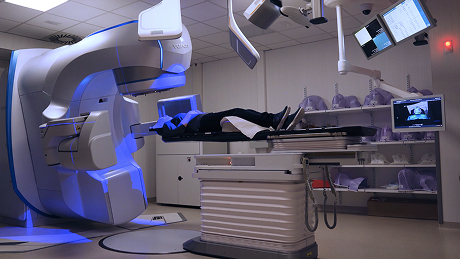
In 2022, Peter was transferred to the Department of Radiation Oncology at Ludwig Maximilian University (LMU) in Munich. From February 2022 to February 2024, more than ten brain metastases were treated across five sessions using stereotactic radiosurgery, a highly precise form of radiation therapy. The metastases are located with millimeter-accuracy using advanced imaging. Then, radiation beams are directed at the tumor from multiple angles, focusing the dose precisely on the target. The energy converges at the tumor site, while surrounding tissue is largely spared.
Several metastases can be treated at the same time, which makes the experience less stressful for patients. “It usually doesn’t take more than half an hour,” says Peter. “And afterward, you can go straight home.”
The fact that Peter needed repeated radiation treatments for brain metastases is—paradoxical as it may sound—also a sign that his therapy is working. “New brain metastases can only form if you’re still alive,” he says.
For the medical team, each new round of treatment brings added complexity—previous radiation sessions and possible interactions with medication all have to be taken into account during planning. “I do realize it’s medically pretty complex,” Peter says. “And I think what they’re doing at LMU is really advanced.”


It’s been over a year now with no new brain metastases. “And my brain’s still working,” Peter adds with a grin. It’s a good thing, too, because it’s had plenty to do lately. “In summer 2024, I was back to working about 40 hours a week,” he says, developing the Titanic exhibition—coordinating content while writing scripts and helping bring them to life.
A full-time job—suddenly interrupted at the end of the summer. Radiation necrosis begins to cause problems. It’s a possible late effect of earlier radiation treatments, in which dead tissue in the brain leads to swelling. The swelling presses on an area of the brain responsible for controlling the left side of the body. For Peter, it’s mostly his left leg that’s affected. “I kind of just dragged it along,” he says. “And I couldn’t really move my hand well either.”
He undergoes surgery in mid-September. The swelling is removed. “I’ve got a titanium plate in my head now—which kind of fits the Titanic theme!” says Peter with a laugh. But in fall 2024, the outcome is anything but certain. At the Lokschuppen, his colleagues start redistributing his responsibilities. His son asks if he should cancel his wedding. “I called the Lokschuppen from the hospital and told them I could still do my job,” Miesbeck says. “And two weeks after the surgery, I was dancing at my son’s wedding.”
Peter Miesbeck knows he’s often been lucky over the past five years.
“The systemic therapies worked well, the swelling was successfully removed—it all could have turned out very differently.” Still, he does a lot to support the effectiveness of his treatment: staying active, eating mindfully and no more alcohol. “I haven’t quit smoking yet,” he admits, “but that’s next on the list.”
Other than that? For now, Peter isn’t planning any new exhibitions.
As an honorary member of the museum’s supporters association, Peter Miesbeck’s advice and perspective will continue to be valued at the Lokschuppen Rosenheim.

But one thing won’t be the same as before: Back when he was running the Lokschuppen, Peter always hoped for rainy school holidays—the perfect conditions for high visitor numbers. These days, he’s happy when the weather’s good.