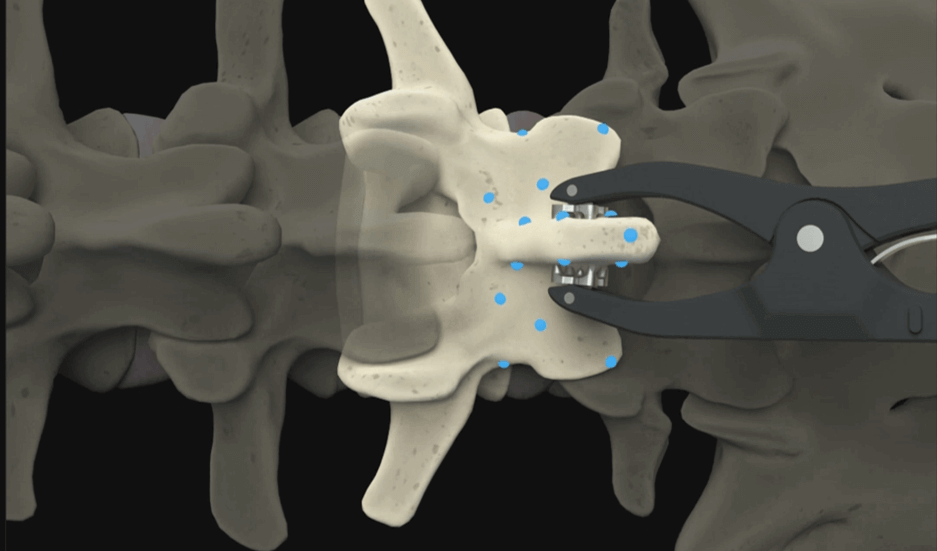
Image registration correlates digital patient images with the actual patient during surgical navigation. Many different modalities can be fused, all contributing to the goal of greater accuracy. The steps involved to complete image registration to begin navigation are preoperative planning, intraoperative image acquisition, combining pre- and intraop images and finally patient registration.
Image registration is an important step in completing a procedure with a surgical navigation system. Also sometimes known as patient registration, image registration is a process used to correlate digital patient images on a surgical navigation screen with the exact, actual position of the patient on the table. There are various processes and devices that can be used to register the patient, but the goal is the same: To achieve high precision surgical results.
Image registration, sometimes called patient registration, is used to correlate patient scans with the patient on the table before and during surgical navigation.
Image registration: Step-by-step
The ultimate goal of image registration is to have a dataset or image of the patient align perfectly with the intraoperative position of the patient. This means that the dataset shown on the navigation screen is equal to the patient’s position on the table in real time and space. You get to that result by identifying points on the dataset and then identifying the same points on the patient’s anatomy to confirm the match.
In automatic image registration, the intraop imaging device itself is equipped with a reference array. A reference array is a clamp or other device equipped with reflective elements in a set configuration that can be recognized by the navigation camera. A second array is attached to the patient’s anatomy. When the scanner sends the image to the navigation system, the exact location of the patient is already determined thanks to the arrays and the surgeon can then verify the registration accuracy.
Step 1: Preoperative planning
Before surgery, you may have preop images that your patient has brought with them. Even though you didn’t personally acquire these images, there’s a lot you can do with them using planning tools. Plan screws or trajectories, segment the anatomy including vertebrae and critical anatomical structures, such as the spinal cord, or outline specific structures like a disc space or tumor.
Step 2: Intraoperative image acquisition
Intraoperative imaging has been a buzz word in the spine community of late for many reasons. More and more, surgeons are looking for quality and flexibility when acquiring images in the operating room. Intraop images provide the surgical team with real time information updates on the patient’s location and the surgical situation.
Types of imaging modalities for image registration
In spine surgery, several different image modalities can be used to plan and navigate common and complex cases.
MRI — Allows for identification of soft tissues and is commonly needed for tumor resection. If the hospital doesn’t have an intraoperative MRI, this scanner will most likely be located in the radiology department.
CT — Ideal for visualizing bone and is more commonly available as an intraoperative device than MRI scanners.
XT (cone beam CT) — The most common intraoperative imaging devices (like 3D C-Arms or angio scanners), XTs are generally less expensive than CT and MR scanners while still providing quality sufficient for bone definition.
Step 3: Combine pre- and intraop images
The next step is to bring preoperative and intraoperative images together. This is accomplished by fusing them together with image fusion software. There are several modalities you can fuse: MRI and CT, CT and CT, CT and XT and MR and XT. Depending on the indication, you may need either rigid or elastic fusion. To learn more about image fusion, please read our Journal article: How Image Fusion Supports Surgical Decision-Making.
Step 4: Patient registration
There are two basic ways to register the patient to the navigation system: Manual and automatic image registration.
Automatic image registration is possible when the scanner is equipped with a reference array or markers. A reference array is also attached to the patient, and their position is thereby identified as they are scanned. The images are then sent automatically to the navigation system and the patient is registered. At the end of this process, a verification step allows the surgeon to confirm the registration. Automatic image registration is ideal for teams that can benefit from less active steps, as it can enable faster and more efficient workflows without much additional effort.
Manual image registration can be obtained by matching points on a preop dataset to the patient positioned on the table. Often these points are planned and acquired on accessible anatomical landmarks. Using manual registration requires a bony surface, such as the spinous process or vertebral laminae, to be visible and accessible. By mapping the posterior surface of a vertebra with a pointer, the navigation system can match the orientation and exact position of the patient to the preop image. This method is useful for cervical cases, most of which are open surgeries with access to the vertebra, and also for re-registering a patient after moving the patient reference, often without the need for additional scans.
Manual registration is also a quick process, but as the name suggests, requires a few more active steps. One major advantage of manual registration is that it can decrease radiation to the patient and team, since less scans may be required.
Step 5: Surgical navigation can begin
Once the registration, either automatic or manual, has been verified, the surgeon is free to proceed with navigated surgery. The flexible nature of the spine can increase the risk of movement and thereby inaccuracies, making navigation essential for maintaining accuracy. Gaining access to increased accuracy in spine surgery can be achieved in just a few simple steps with image registration.
Since there are several registration options available as outlined above, it’s important to look at your case load and choose the best method for you, your team and your patients. Tailoring your workflow with the correct registration method may in turn increase your O.R. efficiency, reduce unnecessary radiation exposure to everyone in the room, and improve outcomes for your patient due to higher accuracy through navigation.