网络研讨会
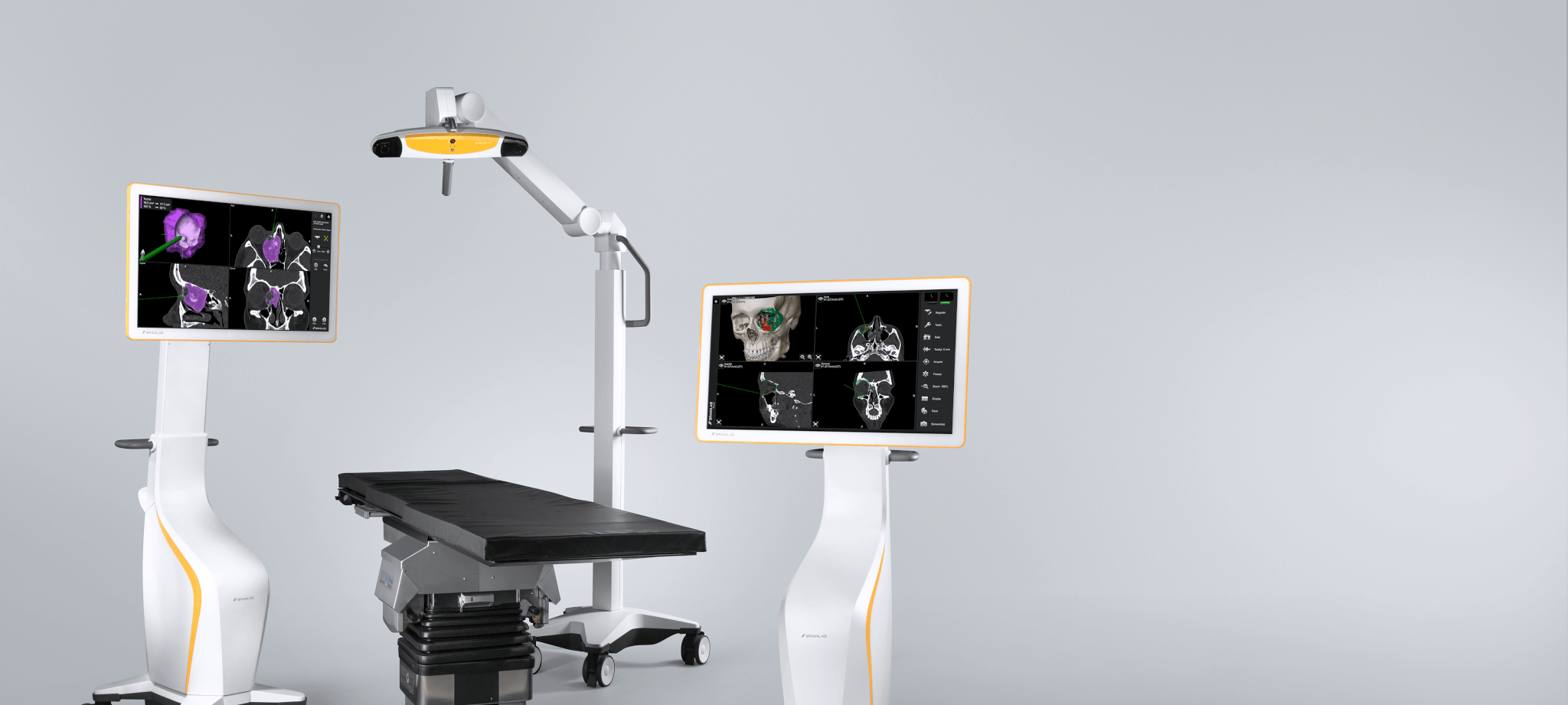
Patient-matched Total Temporomandibular Joint Replacement with Intraoperative Real-time Navigation and Intraoperative 3D-imaging
说明
Brainlab invites you to join our live webinar, “Patient-matched Total Temporomandibular Joint Replacement with Intraoperative Real-time Navigation and Intraoperative 3D-imaging”, on September 29, 2020 at 4:00 PM CEST presented by PD Dr. Dr. Rüdiger Zimmerer, DMD Department of Oral and Maxillofacial & Plastic Facial Surgery University Hospital Leipzig, DE.
This webinar will cover topics including:
Simultaneous intraoperative real-time navigation at mandible and lateral skull base
Registration methods
Trajectorial planning
Real-time guidance of instruments (Calibration matrix)
Intraoperative 3D imaging (fusion of plan and outcome)
Total Joint Replacement with patient-matched prosthesis
Keypoints of virtual planning of TJR
Indications & Limitations
Contralateral sagittal split and Le-Fort-I osteotomies
We look forward to meeting you online!
Language | English
In case you can not join the webinar, it will be recorded and shared afterward.
Participation is free of charge.
发言人:

Rüdiger Zimmerer, 双博士学位
德国莱比锡大学医学中心
查看更多即将举行的网络研讨会
Discover more