The old adage “Time is money” is especially true when it comes to construction projects. From skyscrapers to home improvement projects, any set back can start a chain reaction of delays. And every delay costs time, which means they can also be very expensive. The same is true for integrated operating room projects; Regardless of how thoroughly they are planned, unforeseen hiccups can result in time and money lost.
In the case of designing and building a project as complex and critical as an operating room, planning with a blueprint may not be enough to properly determine the best layout and functionality for the entire O.R. team. Many hospitals that are about to build new operating rooms, especially large scale facilities with multiple O.R.s, are opting instead to first build mock O.R.s to test the equipment and workflows in a real-life setting.
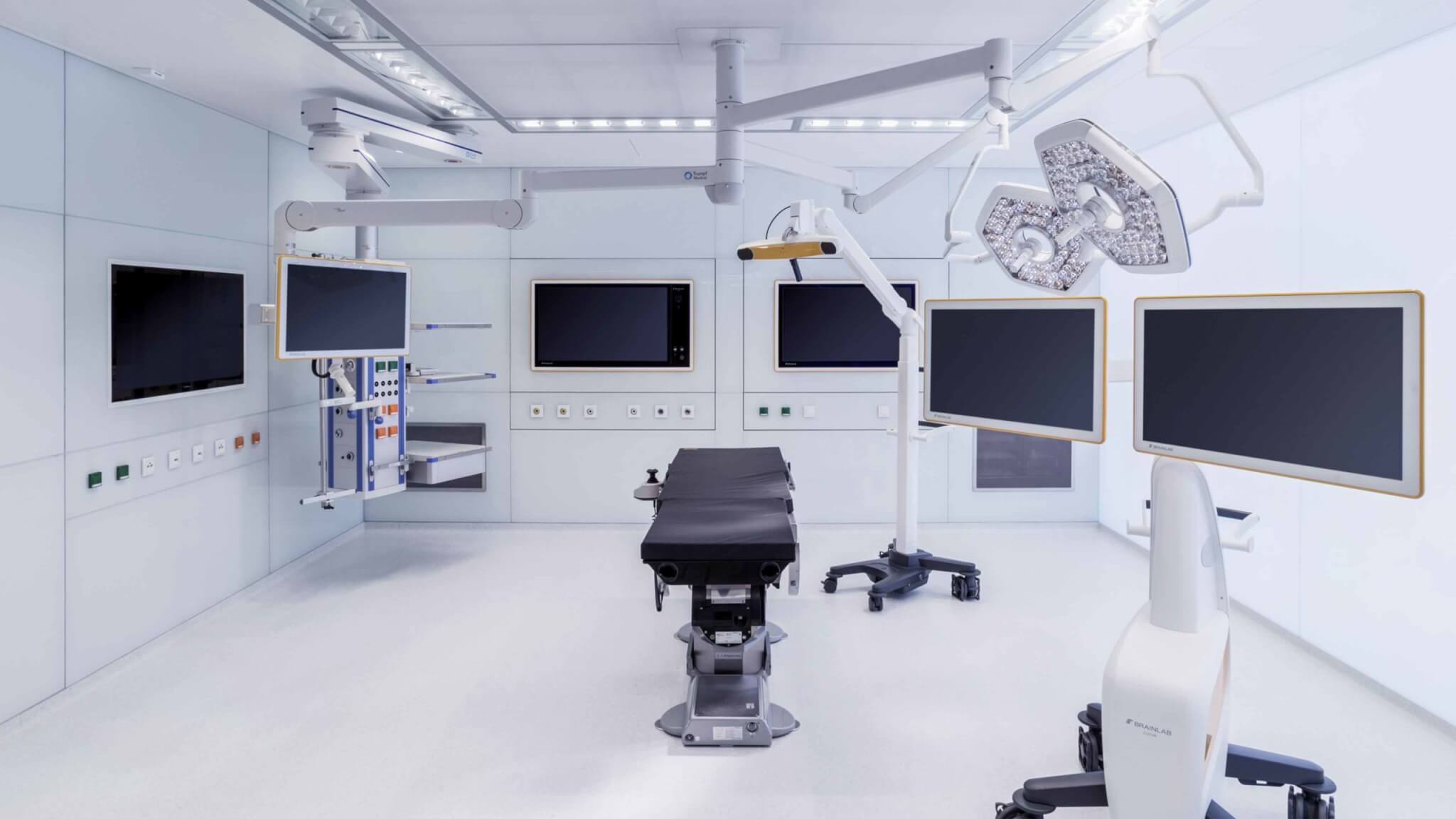
Simply put, a mock O.R. is a non-clinical replica of a real operating room. It contains all the equipment that one might need to treat a real patient. The goal of a these simulated operating rooms is to provide the members of a surgical team with an environment in which they can test out different technologies, software and setups in a realistic environment before construction begins.
A mock O.R. offers the team the perfect chance to establish what they need to incorporate and where elements, such as cabling, breakouts, switches, displays, equipment, ceiling-mounted devices, etc. should be placed. In addition to physical components, these O.R.s also allow for the software that will be integrated to be tested, including the network that will support the various applications. Establishing all this beforehand can therefore make construction a much smoother process.
These kind of simulated operating rooms can be financially very beneficial to hospitals, especially when multiple O.R.s are being built. Establishing the desired setup and configuration in advance reduces the risk of mistakes during construction. We’ve seen cases in which elements that had already been installed had to be torn down and rebuilt, cabling had to be pulled and progress halted. Imagine the cost in discovering too late that one element installed in 20 new operating rooms is incorrect and needs to be redone! Using a mock O.R. to perfect the plan can therefore be essential to avoiding these kind of errors during construction.
After construction, time saving will ideally continue when the operating room goes into clinical use if a mock O.R. is used to select the correct technologies. Filling out the surgical checklist, for example, might take 12 minutes if done on paper. The nursing team may test a digital surgical checklist and discover that it only takes them five minutes to complete the same task, thereby informing their decision. Choosing the right configuration of systems—one that has the potential to shave minutes off surgical time—can therefore save the hospital significant funds in the long run.
In addition to being built at hospitals in the pre-construction phase, mock O.R.s also exist at educational institutions, within specialized mobile vehicles, as well as at companies that build and provide technology for operating rooms. So why not just send members of the O.R. team to one of these locations to test out the technology instead of spending the time and money to construct one in the hospital?
First of all, by visiting an external mock O.R., the team is limited by what is available in that particular setup. There is no flexibility to incorporate the technologies the team may be interested in. There is also no possibility to test the setups as envisioned by the hospital to see if they indeed work. Testing in full scrubs and gloves is also important to understanding how the team’s attire may impact the way they work in the surgical environment.
Secondly, the entire team may not be able to visit an external O.R. Even if they could, they would be limited by time. Allowing all members to test out the O.R. setup is especially crucial in cases of entire newly constructed O.R. departments, since there can be upwards of 300 nurses who will be working in and around the rooms. The feedback is therefore more comprehensive if nurses, surgeons, teaching and support staff are all able to access and test it.
All this begs the question: Where should a hospital create a mock O.R. to provide the surgical team access to it? The hospitals we’ve worked with have always gotten creative when it comes to choosing the location. In some cases, old facilities were being torn down to accommodate new ones, so mock O.R.s were constructed in these soon-to-be demolished buildings. In other cases, hospitals converted unused areas like patient or training rooms. In a few cases, some of our customers even temporarily sacrificed an existing operating room to test out their desired future setup.
New operating rooms projects are often dictated by tenders. The hospital’s end users don’t always get a say in the decision-making process. While the O.R. team is focused on the clinical need, the tender might not include technology that will improve the work of the operating room staff. A welcome side effect of constructing a mock O.R. in-house can be a boost in team morale. If every team member can provide their feedback, especially the nurses who are rarely consulted about technology and setup, then every member feels like a valuable contributor to their future operating room. Constructing these simulated operating rooms is an excellent way to generate excitement among all users at all levels before the project is even complete.
Mock O.R.s are a great proof of concept that are sure to save the hospital time and money both during and long after construction.