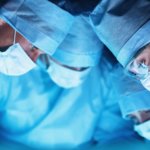
5 Big Trends in O.R. Digitalization
Brainlab has identified five trends in digital operating room integration that are here to stay: Speech control, automation, forward-looking infrastructure, simplicity and the digital twin.
In every area of business, digitalization has become an essential part of staying relevant. The same shift is happening in the healthcare industry, as we’ll be exploring through posts on this blog. Disruptive technologies will continue to push boundaries and change the way O.R. teams administer surgical care. A lot of trends are on the horizon, but which are here to stay? Check out our predictions below.
1. Speech Control
Today, most high-tech systems in the O.R. are touch-controlled. With new, touchless methods of software control being developed for every day devices, the future of the O.R. will also offer the surgical team new ways of interacting with devices and software.
The sterile field in the O.R. is essential for protecting the patient from potentially life-threatening pathogens. Offering the surgeon the possibility to control devices and software without having to leave this field, keeping their hands free to operate on the patient, will have a huge impact on outcomes and patient safety. Existing touch-based technologies to address software within the sterile field include draped ceiling-mounted and handheld displays. In the near future, however, touchless solutions, like gesture recognition, eye tracking and speech control, will enter the O.R.
Gesture recognition can be inefficient and even counterproductive, since it takes the surgeon’s hands away from the patient. Bright O.R. lights can interfere with the correct interpretation of hand movements. At this point, the variety of gestures as commands is limited and the technology as a whole still requires a lot of development. Addressing some of these potential issues is eye recognition, which quickly identifies the user’s field of view. While completely hands-free, this method is still fairly inaccurate and suffers from the “Midas Touch problem”: Involuntarily triggering actions by accidentally looking at the controls 1.
In terms of what methods of hands-free control will present the fewest problems in the surgical field, we believe speech recognition has huge potential to become a mainstay in the O.R. Through speech command, the surgeon can give orders, for example, to zoom in or out from a displayed view from across the room, to change the content showed in a display, to record a video, or to conference in a colleague outside of the operating room. Their usual surgical workflow wouldn’t be impacted, as it would be as if they were asking a nurse to perform the desired action.
The technological challenge with speech control is to develop improved voice recognition software using more natural commands that also minimizes background noise to rule out false commands. More natural commands could also potentially increase system usage. Underuse is a problem we’ve observed with many of our customers: They have great technology, but it’s not being taken advantage of because the team doesn’t know how to use it. Simplifying the way the team interacts with their software could therefore also increase usage and streamline training.
While Siri, Google Home and Amazon Alexa have made speech control an everyday reality for many, we believe that speech control will also play a significant role in the O.R. of the future.
2. Automation
The age of digitalization offers many more opportunities for automatization than ever before. With the marriage of IT and operations technologies, intelligent devices are already totally transforming whole industry processes and business models. The hospital environment also has the potential to achieve a higher degree of automation. Surgical workflows especially, which are still made up of a wide range of mostly manual tasks, can gain enormously from automation.
Sterile workflows in the operating rooms are, in fact, already being optimized by improved processes based on visual identification, for example, with Steri-ID trays that distribute sterile equipment to the right place at the right time. Patient data is also already be transmitted when needed before surgery even begins based on HL7 message standards. Even O.R. management is taking steps in this direction, with multiple vendors in the market working on tracking and automating processes for their workflow steps. Research institutes are thinking about how to automate workflows in an operating room as well, like OR.net, a collaborative project initiated by ICCAS institute at Leipzig University, Germany5. OR.net aims to build an open infrastructure by standardizing processes and opening it up to automation by using standard internet protocols, such as WSDL, SOAP, and XML Schema.
So will we see a “Smart O.R.” in which self-learning devices work and sync autonomously anytime soon? In order to achieve this vision, it is crucial to take the first steps towards digitalization now, starting with hospital infrastructure to create the foundation for the operating room of the future.
3. Infrastructure for the future
Internet Protocol (IP)—the way in which data is sent from one computer to another over the Internet—actually builds the foundation of all of the above listed “smart” developments. IP is being used more and more widely for voice and video over IP, but also for information exchange between devices, aka the “Internet of Things”. All devices’ sensors get an IP interface and are thereby connected to one IP hub. Devices form a whole network in which data is exchanged continuously in order to improve collaborative work. Using the open, standardized communication of such IP-networks can bring huge benefits to the hospital, like efficient data exchange to and from the O.R., the elimination of “cable spaghetti”, as well as the possibility to interconnect unlimited numbers of medical devices with just an IP address.
4. Simplicity
You might wonder why simplicity in the O.R. is a trend for us, as it should be obvious that this is something every industry should strive for. For us, simplicity ultimately leads to productivity and effectiveness. The goal of technology should be to simplify the way users work to achieve greater productivity.
Unfortunately, this is not always the case. Taking all the above-mentioned trends into account, one can clearly see that complexity is also increasing. Setting up a digital O.R. environment with deep IT integration based on IP-solutions and implementing a Hybrid O.R. might seem overwhelming at first glance. But taking a deeper look into each of the four trends, it becomes clear that despite a high degree of complexity in the O.R., they all have the potential to simplify specific workflows. All IP-solutions achieve efficiency by simplifying data transfer and eliminating cumbersome service. Speech control enables simple device handling from the sterile field. Automated data transfer and O.R. management workflows will save time. Hybrid O.R.s, where surgical results can be verified intraoperatively and improved if needed, will help prevent complications and further hospital visits, therefore resulting in highly effective surgical procedures.
5. Digital Twin
Throughout the entire patient journey, a massive amount of unstructured data is created—from pathology, blood tests, and images, to name a few. To use this data to its full potential, a digital twin—also known as a virtual model—of the patient can be created by structuring and analyzing the data. That digital twin is then stored in the patient’s Electronic Medical Record (EMR) and can be expanded over time as more data is amassed, helping to streamline workflow processes along the entire patient journey.
While the concept of a digital twin is not new, originating in manufacturing, we’ve seen their potential quickly growing in the healthcare field. In the future, it may be possible to incorporate statistical information, such as typical outcome of a specific procedure, to create an optimal patient treatment plan. By having all the information collected about a patient in one location, surgeons can streamline their clinical workflows. When it comes to surgery specifically, digital twins can give clinicians more information about the patient and, when combined with statistical information, can hopefully support improved treatment outcomes.